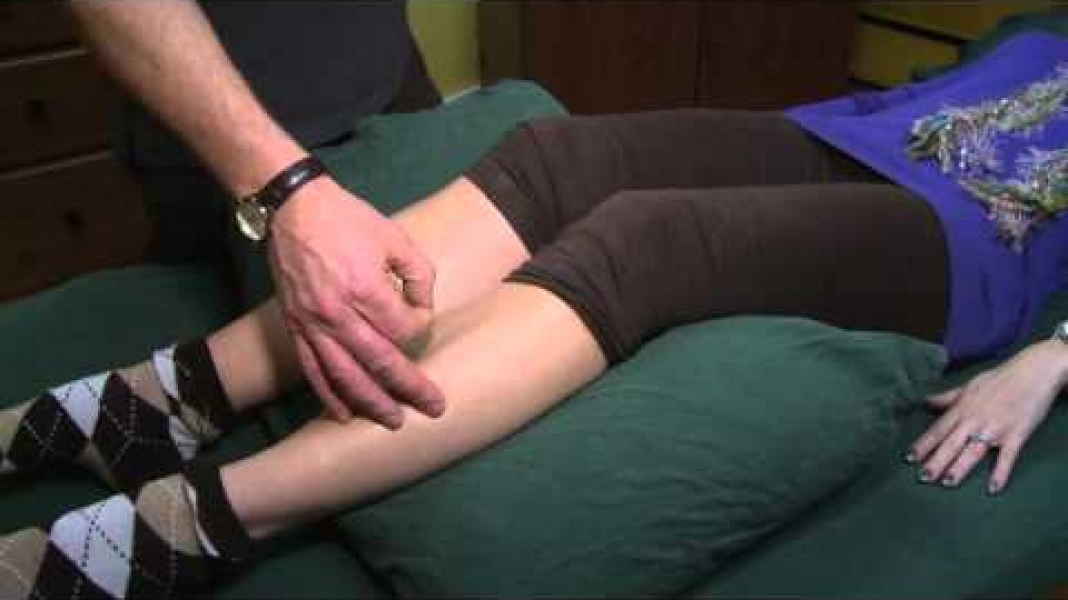
There can be many reasons. Here is one typical problem we see where regular stretching is not therapeutic and can make things worse. There is a natural curve in the lumbar region of the spine (called a “lordosis” in physio talk). When our back is in this normal curved state it is called the “neutral position”. Many modern jobs demand people sit all day causing the lower back to be chronically and excessively bent forward in an “unnatural way”, out of neutral position. Also, some physical jobs demand a person to bend forward for long periods of time or in repeated lifting sequences. This can cause the lower back to be over-loaded in a “flexed” or bent forward position. Many with back pain regularly stretch their back muscles routinely at work, at home or in yoga classes, because it feels great and relieves the pain. But, If you are doing this type of back flexion stretching, it may be re-stressing your already over-loaded and over-sensitive vertebral discs and joints.
This blog is about why you may be making things worse in the long run with stretching your back and/or hamstrings, and how to shift your focus away from stretching and toward a better strategy of proper muscle activation. This does not involve intense core strength training or going to the gym necessarily…..
The lower lumbar section of the back is designed to have limited mobility and to be loaded in a “neutral” lordosis or natural, inwardly curved position — not flexed and bent outward under loading. You can do it, but you eventually pay the price! Your back muscles can tighten, likely a response to protect your lower back structures by pulling it out of flexion – these muscles become overworked and spasm sometimes. That’s where our Edmonton acupuncture clinic comes to rescue! You visit us and we reset the back with acupuncture. Before we send you on your way, we teach you about how stretching the low back muscle triggers a neurological reflex that reduces your back’s pain sensitivity for a short time (15-20 min). We show you how you may be aggravating the problem after this temporary relief, and the pain not improving or may even return worse than before. So the solution for people with chronic lower back pain is to NOT stretch the lower back, but rather to focus on maintaining the back’s neutral position as much as possible in rest and work and play, in normal movements throughout the day, and in rehabilitative exercises!
So the primary problem is not with your back muscles per se. More often than not, lower back pain is the accumulation of years of functional wear and tear on your vertebral discs and joints at work or play, leading to small accumulations that become bigger issues later. Once the last straw has been placed on the camel’s back, and the pain has arrived. Over 10% of adults suffer with chronic back pain, and many more suffer back pain at some point in their life. Well intentioned people can make their back worse by over training certain muscles in the wrong ways, not finding the right balance of strength and length for the right places. And there are many myths that perpetuate problems of back pain, especially in our system of medical diagnosis and treatment, and how common treatments may not always offer good solutions for your particular problem.
This blog helps to offer insights for you to better understand the particular nature of your back problem, and then to functionally address your recovery systematically and strategically. The way information is presented here comes mainly from what we have learned from the research and very practical recommendations of back pain expert Dr. Stuart McGill. He is recognized internationally as a guru in back dysfunction, and is a professor of Spine Biomechanics at the University of Waterloo. McGill has explored the nature of lower back function and pain for over 30 years, publishing over 400 scientific papers and several text books. McGill has developed strategies for injury prevention and rehabilitation based on cold hard scientific evidence and the experience with applying practically what he has learned to functional rehabilitation programs. He has been able to help many whose problems were not properly assessed and treated from a functional perspective, who had given up hope, told they had to learn to live with the pain, and were reliant on pain medications. McGill also has learned a lot by helping many Olympic athletes overcome their back pain, who then have gone on to achieve their best performances and reach the podium.
One of McGill’s big myth busters is that back Xray or MRI pictures provide the doctor with what they need to know in terms of your course of treatments. It is as if once we have the picture showing something out of place the doctor knows what to do. He says these images may prove useful once surgery has been determined to be the only remaining option (which is extraordinary), but in the beginning, in and of themselves, they may be unnecessary or only a small piece of the puzzle in treating someone functionally. Many have bulging discs or degenerative vertebral processes but no pain, so when we see these phenomenon medically, they should not necessarily indicate the treatment (by drugs, exercises, rest).
Repeated flawed movement patterns are the cause of back issues that can make them sensitive to the slightness load. The medical examiner (or you) should be focusing on what triggers that pain functionally, then from this develop a more strategic and responsive rehabilitative plan based on functional improvements. McGill says “if you ever have pain-free movement, you have the capability to expand your repertoire of pain-free movements to become pain-free living. You are curable”. McGill’s recently published book, “Back Mechanic”, is a wonderful practical guide to help people become their own back mechanics, responsive to the nature of their own problems, both in developing better practices in their daily lives, but also in working with their doctors, physiotherapists, and other health care practitioners like us at The Acupuncture Turning Point.
McGill also says, “If your Doctor’s primary approach to your recovery lies in pain medication, you need different expertise”. He says, “If all you have been given is a list of exercises from your physiotherapist, you need to find a new approach”
And along these lines, I feel confident to say he would agree with my thought, that if all you get is acupuncture for back pain from your acupuncturist, adjustments from your chiropractor, or massage from your massage therapist, and you need repeated visits just to manage your back pain over the years, your need to find a new way! When you see us at The Acupuncture Turning Point we speed up the process of you finding a better approach. We know that acupuncture or other therapies for back pain are assisting you on that journey, and do not cure you of your problem by themselves.
We sell McGill’s practical guide “Back Mechanic” at cost at our clinic ($40 + GST), or you can buy it online from the usual outlets like amazon. In the meantime, if you don’t get the book, watch for our series of blogs in the next year on back pain, where we summarize the highlights of this practical reference.